
 Revenue Cycle Management
Revenue Cycle ManagementWhat are Mandatory Medical Billing Compliance Rules for Practices in 2026?

Content
Medical billing is driven by strict compliance rules. These rules have been introduced primarily to standardize how bills are generated and submitted. A compliance-driven billing guarantees accuracy, integrity, and ethical practices. Likewise, it helps to prevent fraud, abuse, and patient privacy violations.
For healthcare providers, adhering to compliance rules brings in several benefits. It is a cornerstone to efficient revenue cycle management, improved patient satisfaction, and overall operational efficiency.
This blog will explore the various mandatory medical billing compliance rules that practices must follow to ensure smooth billing operations.
Understanding Medical Billing Compliance: Importance and Example
Medical billing compliance refers to the adherence to laws, regulations, and ethical standards in the process of submitting medical claims for reimbursement. It ensures that healthcare providers, billing professionals, and organizations follow proper procedures when submitting claims to insurance companies or government programs like Medicare and Medicaid.
For example, a healthcare provider must ensure that the codes used for diagnoses and procedures (such as ICD-10 or CPT codes) are accurate and correspond to the services rendered. If a doctor provides consultation for a patient with a specific condition, they must use the correct codes related to that condition, ensuring that no overcharges or fraudulent claims are made.
Failure to comply with medical billing regulations can result in penalties, fines, and even the loss of the ability to bill for services. By maintaining medical billing compliance, healthcare organizations help ensure ethical practices and safeguard against fraud.
Medical Billing Compliance Rules for Practices
Some of the mandatory medical billing compliances are:
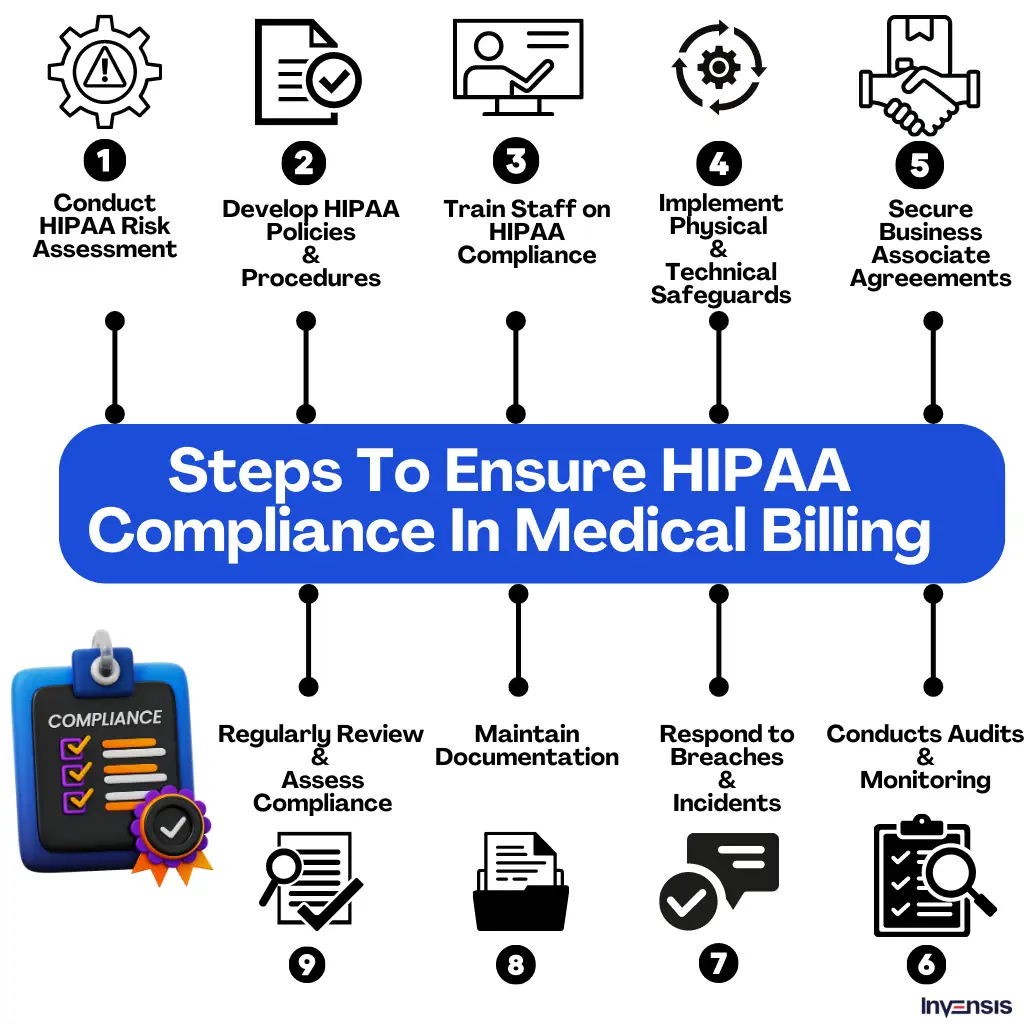
1. HIPAA Compliance Rules
The Health Insurance Portability and Accountability Act (HIPAA) is a federal law in the United States that safeguards the privacy and security of patients' protected health information (PHI). It sets standards for electronic transactions, requires safeguards for PHI, and grants patients certain rights regarding their health information.
These rules mandate the use of standard electronic transactions, such as electronic claims submission, to protect the integrity and confidentiality of patient data. Healthcare practices must obtain patient authorization for disclosing PHI, except in certain permitted circumstances. HIPAA also grants patients the right to access and obtain copies of their medical records. Practices are required to maintain detailed records of PHI disclosures and implement administrative, technical, and physical safeguards to maintain privacy and prevent unauthorized access or breaches.
Protected Health Information (PHI) refers to any individually identifiable health information transmitted by a covered entity or business associate. In medical billing processes, It includes patient demographic details, medical history, treatment records, insurance information, and payment details. Handling PHI in billing requires strict adherence to HIPAA rules. Practices must ensure secure transmission, limit access to authorized personnel, use encrypted systems, and employ measures to prevent unauthorized disclosure.
2. Coding Compliance Rules
Coding compliance in medical billing refers to the adherence to established coding guidelines and standards, such as using accurate Current Procedural Terminology (CPT) codes and International Classification of Diseases (ICD) codes. It ensures that coding is consistent and accurate and supports the medical services provided, enabling proper billing and reimbursement.
The Current Procedural Terminology (CPT) coding system is a standardized set of medical codes used to describe medical procedures and services provided by healthcare professionals. Developed and managed by the American Medical Association (AMA), CPT codes are essential for accurate documentation, billing, and reimbursement in medical practices, facilitating efficient communication between healthcare providers and payers.
The International Classification of Diseases (ICD) coding guidelines provide a standardized system for classifying and coding diagnoses, symptoms, and procedures. These guidelines ensure consistency and accuracy in medical documentation, enabling effective communication, statistical analysis, and reimbursement processes across healthcare systems and providers globally.
Maintaining coding accuracy plays a crucial role in medical billing compliance. Errors in coding can lead to claim denials, delayed reimbursements, or even allegations of fraud. Incorrect codes may result in overbilling or underbilling, both of which can have financial implications. Accurate medical coding ensures that the services rendered are properly documented and billed, aligning with coding guidelines. By maintaining coding accuracy, healthcare practices can enhance billing compliance, reduce errors, and optimize revenue generation.

3. Fraud & Abuse Prevention Rule
Fraud in medical billing refers to deliberate deception or misrepresentation of information to obtain unauthorized financial gain. For example, billing for services not provided or performing unnecessary procedures. On the other hand, abuse refers to practices that deviate from acceptable healthcare standards, leading to high costs without intentional deception, such as unbundling services or upcoding.
The False Claims Act (FCA), the anti-kickback statutes, and the Stark law come under fraud and abuse prevention rules. The FCA imposes liability on individuals or entities that submit fraudulent claims to the government for payment. Healthcare providers can face substantial penalties, including treble damages and fines if found in violation.
The Anti-Kickback Statutes prohibit offering, receiving, or soliciting anything of value in exchange for referrals or generating federal healthcare program business. On the other hand, the stark law prohibits physician self-referrals for certain designated health services.
Healthcare practices can establish effective compliance programs to detect and prevent fraudulent practices. They should conduct regular risk assessments and implement clear policies and procedures. Also, fostering a culture of compliance and Regularly reviewing and updating the compliance program can help them to stay aligned with evolving regulations and industry best practices.
4. Documentation & Record-Keeping
It is mandatory for medical practices to maintain accurate and comprehensive documentation of patient encounters. The documents must include medical histories, examination findings, treatment details, and other relevant information. The documentation should be timely, legible, and complete ensuring a clear and accurate representation of the patient's health.
Healthcare providers should follow established protocols and document patient encounters using consistent terminology, abbreviations, and formatting. This consistency ensures clarity and minimizes the risk of errors or misinterpretations in the billing process. Besides, healthcare practices should also establish an audit trail for documentation and reporting. This includes the record of key changes or corrections made to the documentation, along with an explanation for the modifications.
As per the above rule, every patient documentation must comply with HIPAAs privacy and security needs. Medical practices must protect patient information and take necessary measures to prevent unauthorized access or disclosure of sensitive data. Healthcare practices should also ensure the proper handling, storage, and transmission of patient information.
5. Billing Audits and Compliance Reviews
Regular billing audits and compliance reviews are vital for ensuring that medical billing practices are adhering to the necessary regulations and standards. These audits help healthcare practices identify discrepancies, inaccuracies, and non-compliance issues that could lead to financial penalties or reimbursement delays. Auditors examine medical records, patient documentation, and billing codes to ensure they are consistent with the services rendered. A well-executed audit process can also help detect fraud or abuse in billing practices, reducing the risk of overbilling or underbilling.
The audit process must be thorough, covering areas such as coding accuracy, medical necessity, and compliance with payer-specific requirements. Conducting audits and reviews at regular intervals allows practices to stay ahead of potential compliance issues and make necessary adjustments before they lead to major violations. Corrective actions, when needed, should be implemented immediately to improve compliance and ensure that the practice remains in line with current regulations. Training staff on compliance standards and auditing techniques is crucial to maintaining an effective audit system.
6. Medicare and Medicaid Compliance
Healthcare practices that accept Medicare and Medicaid must adhere to specific compliance rules set by these programs, which are governed by federal and state regulations. These programs have strict guidelines regarding billing practices, reimbursement rates, and patient eligibility. Compliance with these regulations ensures that providers receive appropriate reimbursement while avoiding penalties for improper claims submissions.
Medicare and Medicaid compliance requirements include accurately documenting the services provided, ensuring that claims are properly coded, and that all relevant services are billed appropriately. Healthcare practices must also follow the program-specific rules on patient eligibility, service coverage, and claim submission timelines. Failure to comply with these requirements can result in claims denials, fines, and even exclusion from the program.
To stay compliant, healthcare providers should stay updated on changes to Medicare and Medicaid regulations, train staff on the specific requirements of these programs, and conduct periodic internal reviews of billing practices. Implementing an effective compliance program that includes ongoing education, documentation checks, and audits will help mitigate the risk of non-compliance and ensure that practices are properly reimbursed for the services they provide.
Conclusion
While following compliance rules is a must, the constant change in compliance rules regarding medical billing introduces complexity to the process. As regulations evolve, healthcare providers must stay updated and adapt their documentation and record-keeping practices accordingly. The introduction of new rules, guidelines, and coding standards requires ongoing training and education for staff to ensure compliance. Implementing changes across systems and processes can be time-consuming and resource-intensive. Moreover, varying regulations across different jurisdictions or insurance providers further complicate the compliance landscape.
The best way to overcome these combined challenges is to delegate medical billing compliance needs to third-party partners. Hiring a third-party service partner can alleviate the burden of medical billing complexities, ensuring compliance with regulations and improving patient care for healthcare practices. We at Invensis, bank on a knowledgeable team of compliance specialists and advanced tech-driven processes to guarantee compliance with all medical rules and regulations. Contact us to transform your medical billing services and make them more compliant
Discover Our Full Range of Services
Click HereExplore the Industries We Serve
Click HereBlog Category
Related Articles

A practical guide for factors to identify invoice fraud, strengthen invoice validation, and protect funding decisions.
May 11, 2026
|
.jpg)
How modern factoring support services empower factoring companies to scale, manage risk, and protect margins amid tightening credit conditions.
April 30, 2026
|

Fix enterprise finances using smart factoring and AI-human collaboration.
April 30, 2026
|
Services We Provide
Industries We Serve





.webp)