
 Revenue Cycle Management
Revenue Cycle ManagementWhat are the Important Components of Medical Billing Workflow

Content
A medical billing workflow is the step-by-step process followed in a healthcare facility to manage the billing and reimbursement of medical support provided to patients. It encompasses the various stages involved, from patient registration to claims submission, payment posting, and accounts receivable management. The workflow ensures smooth and efficient medical claims processing, facilitating accurate billing, timely reimbursement, and effective revenue cycle management.
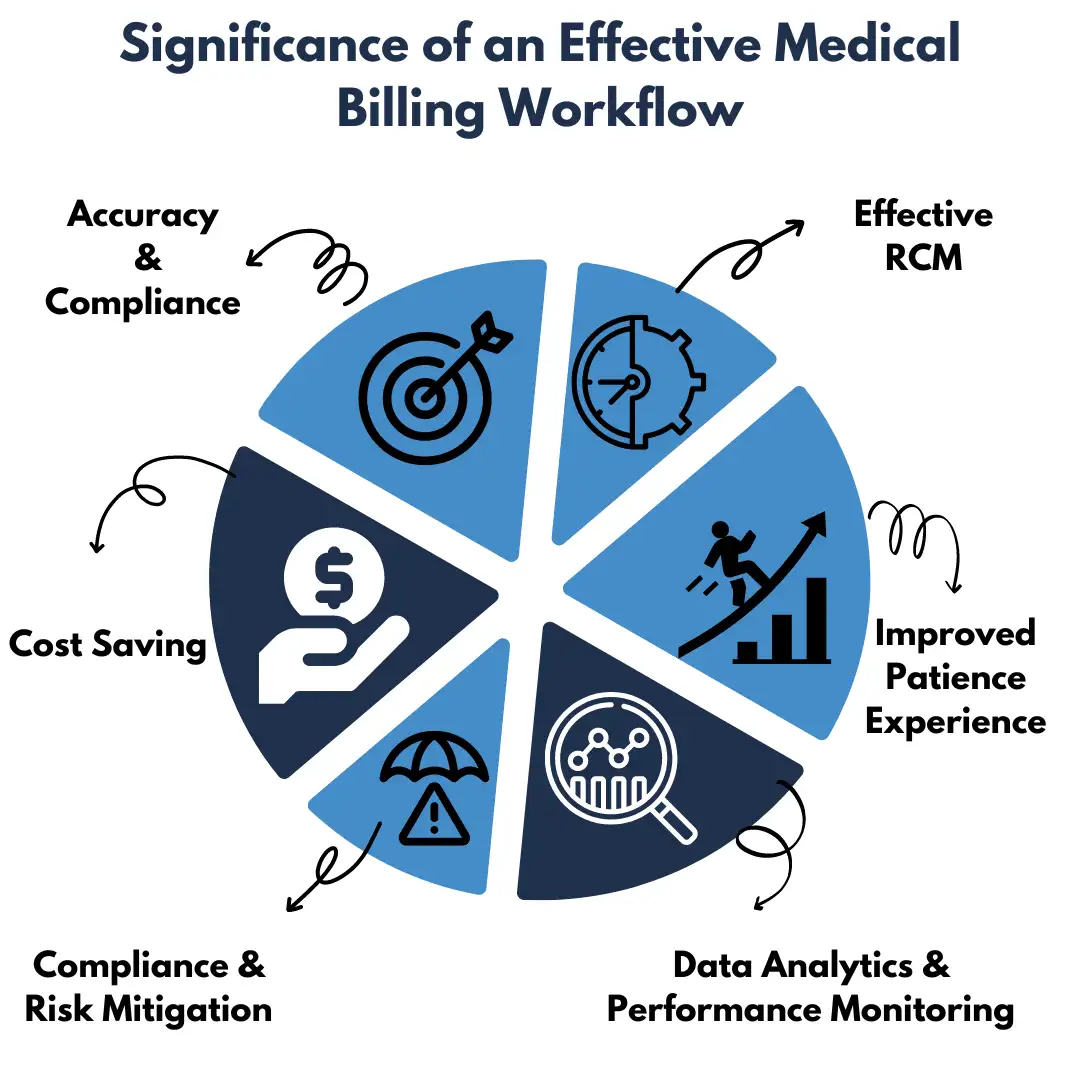
What Are The Important Components of Medical Billing Workflow?
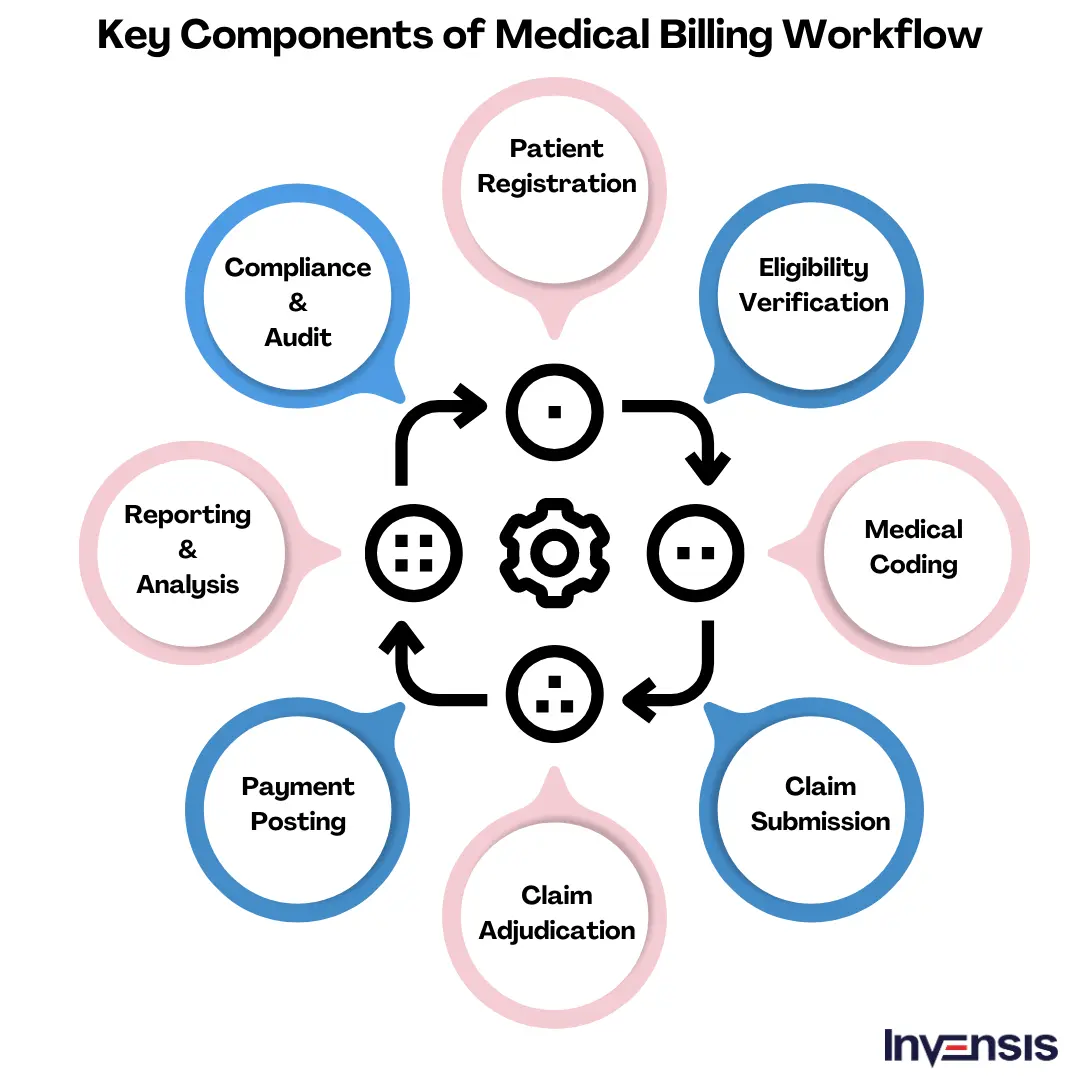
The medical billing workflow comprises several crucial components that ensure accurate and efficient medical claims processing. Each component plays a vital role in the overall revenue cycle management process. Here are the most important components of the medical billing workflow:
1. Patient Registration
The workflow begins with patient registration, where patient demographic information, insurance details, and other necessary information are collected and entered into the system. Accurate and complete patient registration ensures smooth billing processes and facilitates proper claim submission.
2. Eligibility Verification
Once registered, the patient's insurance coverage is verified. This step involves checking the patient's eligibility, coverage limits, deductibles, and pre-authorization requirements. Verification helps ensure that the medical support provided will be reimbursed and minimizes claim denials.
3. Coding
Coding is a critical component where medical procedures, diagnoses, and services are translated into standardized codes (e.g., CPT and ICD codes). Accurate medical coding ensures proper billing and reimbursement by accurately reflecting the medical support provided.
4. Claims Submission
Once the delivered support solutions are coded, claims are generated and submitted to insurance companies or payers. This step involves compiling the necessary documentation, attaching supporting medical records, and submitting the claims electronically or via paper.
5. Claims Adjudication
The insurance company or payer receives the claims and performs adjudication, where they review the claims for accuracy, coverage, and medical necessity. The claims are either accepted, adjusted, or denied based on the evaluation.
6. Payment Posting
After the claims are adjudicated, payment posting is done to record the payments received from insurance companies or patients. This step involves accurately documenting the payment amounts, adjustments, and outstanding balances.
7. Reporting and Analysis
Regular reporting and analysis provide insights into key performance indicators, claim acceptance rates, denials, revenue trends, and other metrics. This data helps identify areas for improvement, track financial performance, and make informed decisions to enhance the billing workflow.
8. Compliance and Audit
Compliance with regulatory requirements, like HIPAA and coding guidelines, is crucial. Regular internal and external audits ensure adherence to best practices, identify potential compliance issues, and mitigate financial and legal risks.
These components work together to form an effective medical billing workflow, ensuring accurate coding, proper claims submission, optimized reimbursement, and streamlined revenue cycle management services. Efficient management of each component contributes to minimizing claim denials, optimizing revenue, and maintaining compliance with industry standards and regulations.
How to Sync the Different Components of Medical Billing Workflow
Most medical practices struggle to build and maintain an effective billing workflow. This is because of reasons like failure to establish clear roles and responsibilities for billing staff and remove kinks from key processes like patient registration, insurance verification process, documentation, claims submission process, etc. To top it, finding qualified medical coders and keeping pace with updated billing rules is a constant challenge.
A proven way to ensure the smooth working of medical billing workflow is by hiring the solutions of third-party partners. They bring expertise and specialized tools that enhance efficiency and accuracy. These partners often provide software solutions that integrate with practice management systems, electronic health records (EHRs), and billing platforms, ensuring seamless data flow between various stages of the billing process. They stay on their toes to keep workflows streamlined, reduce errors, and accelerate reimbursement.
Conclusion
Keeping medical billing workflow streamlined should be a consistent practice to ensure efficiency and productivity. For this, practices must regularly review and optimize processes, foster clear communication, encourage collaboration, and provide ongoing training to enhance skills.
At Invensis, we strive to keep medical billing workflows by adhering to best practices, monitoring performance metrics, and soliciting feedback for continuous improvement. Contact us now to optimize your financial outcomes and elevate your healthcare practice with our efficient medical billing services.
Discover Our Full Range of Services
Click HereExplore the Industries We Serve
Click HereBlog Category
Related Articles
.jpg)
How modern factoring support services empower factoring companies to scale, manage risk, and protect margins amid tightening credit conditions.
April 30, 2026
|

Fix enterprise finances using smart factoring and AI-human collaboration.
April 30, 2026
|
Essential fixes for factoring companies losing money to fraud.
April 30, 2026
|
Services We Provide
Industries We Serve





.webp)