
 Revenue Cycle Management
Revenue Cycle ManagementMedical Billing Trends: The CMS Reimbursement Proposal for FY 2026

Content
In keeping with the practice of updating Medicare payment policies for IPPS hospitals and LTCHs on an annual basis, the CMS has unveiled a proposed rule for fiscal year (FY) 2024. The proposed rule for 2024 introduces changes to payment rates under both IPPS (Inpatient Prospective Payment System) and LTCH PPS (Long-Term Care Hospital Prospective Payment System) along with changes to Social Determinants of Health Diagnosis (SDOH) Codes, New COVID-19 Treatments Add-on Payment (NCTAP) etc.
This blog delves into the key changes as introduced in the CMS reimbursement proposal.
.webp)
Understanding CMS Reimbursement in Healthcare
CMS (Centers for Medicare & Medicaid Services) reimbursement refers to the process by which healthcare providers are paid for services rendered to Medicare and Medicaid beneficiaries. These are government-funded programs that provide health insurance to specific groups, such as the elderly, low-income individuals, and people with disabilities.
Reimbursement from CMS includes a range of services, including hospital stays, doctor visits, surgeries, and prescription medications. The amount paid is determined by CMS through a variety of payment models, which can include:
- Fee-for-Service (FFS): Providers are paid a set fee for each service or procedure performed.
- Prospective Payment Systems (PPS): Payments are predetermined based on factors like the diagnosis or procedure rather than the actual cost incurred.
- Value-Based Care: Payments are tied to the quality of care provided, incentivizing healthcare providers to focus on improving patient outcomes.
CMS reimbursement is a crucial component of the healthcare system in the U.S., ensuring that providers are compensated for delivering care to those covered by Medicare and Medicaid. The reimbursement rates and policies can vary depending on factors such as the type of care provided, the geographic location, and changes in CMS regulations.
Medical Billing Trends: Proposed CMS Reimbursement Rules for FY 2024
Increase in Payment Rates under IPPS
- The proposed increase for general acute care hospitals under IPPS, participating in the Hospital Inpatient Quality Reporting (IQR) and EHR use, stands at 2.8%
- The increase applies to hospitals in the Hospital IQR program and effective meaningful EHR use.
- Such a proposal looks forward to incentivizing quality reporting and EHR utilization for fair reimbursement.
- The payment adjustments incentivize better patient outcomes and care quality.
- CMS aligns payment with performance for patient safety and efficiency priorities.
- The proposed change to increase hospital payments by $3.3 billion in FY 2024.
- Medicare DSH and uncompensated care payments are projected to decrease by $115 million in FY 2024.
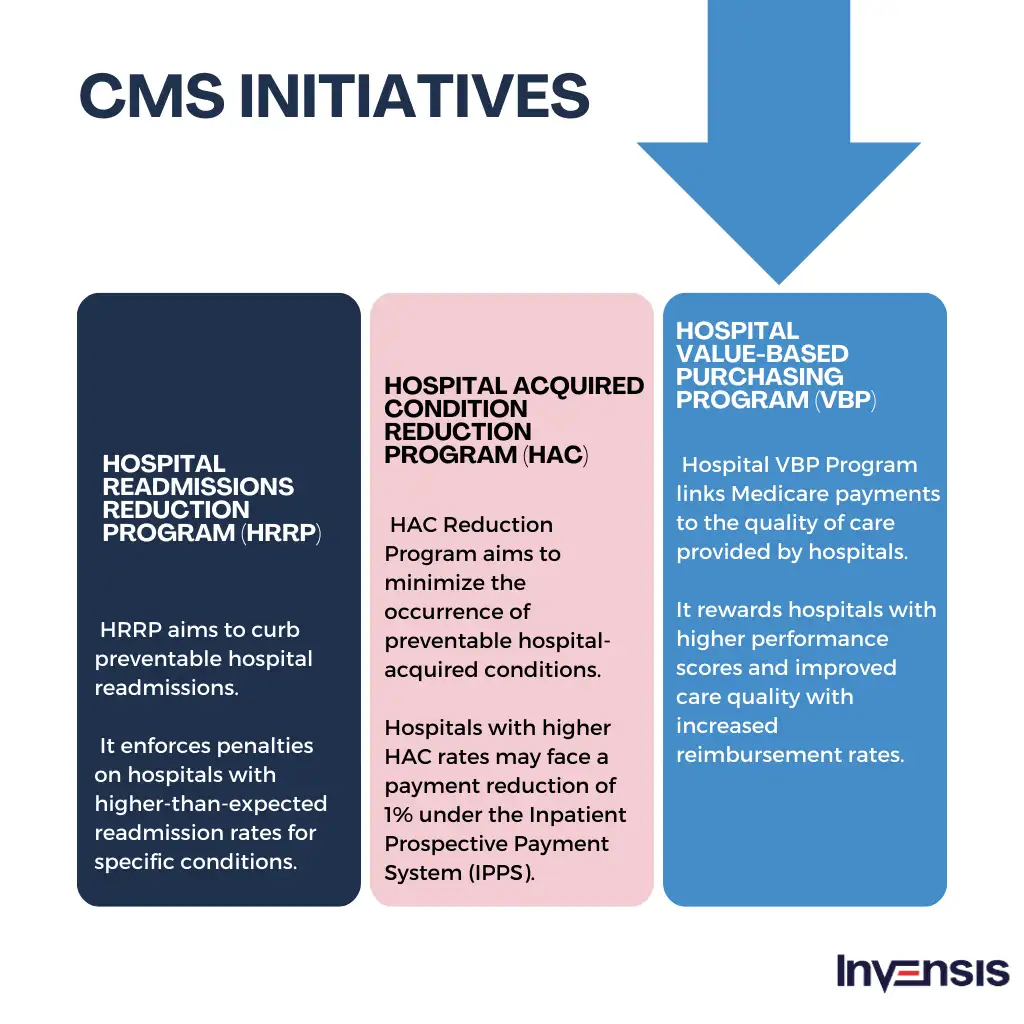
Changes to Payment Rates under LTCH PPS
- CMS projects a 2.9% increment in the standard payment rate for LTCHs in FY 2024.
- LTCH PPS payments for standard rate discharges to go down by 2.5% or $59 million.
- Reduction attributed to a projected 4.7% decrease in high-cost outlier payments as a percentage of total LTCH PPS standard Federal payments.

Medical Billing Trends: Changes to the New COVID-19 Treatments Add-on Payment (NCTAP)
- CMS introduced NCTAP during the PHE.
- NCTAP supports eligible discharges, ensuring continued treatment support.
- To minimize payment disruptions post-PHE, NCTAP extended until PHE's fiscal year-end.
- If PHE ends in May 2023, NCTAP eligibility till September 30, 2023 (end of FY 2023).
- NCTAP expires after FY 2023; no payments from FY 2024 (starting October 1, 2023, discharges).
Conclusion
The new proposed rules by the CMS for FY 2024 hold significant implications for the healthcare industry. The proposed increment in payment rates for healthcare organizations under IPPS will enhance the quality of care, reporting, use of EHRs and ensure equitable reimbursement. At Invensis, we closely monitor medical billing trends, proposed rules and align these with our medical billing services to help practices meet CMS’s vision for FY 2024.
Frequently Asked Questions
Discover Our Full Range of Services
Click HereExplore the Industries We Serve
Click HereBlog Category
Related Articles
How quickly they turn invoices into cash, we break down what really happens inside the invoice validation clock
May 18, 2026
|

A practical guide for factors to identify invoice fraud, strengthen invoice validation, and protect funding decisions.
May 11, 2026
|
.jpg)
How modern factoring support services empower factoring companies to scale, manage risk, and protect margins amid tightening credit conditions.
April 30, 2026
|
Services We Provide
Industries We Serve





.webp)